A medical tool based on night vision technology could help clinicians diagnose lymphatic disorders earlier, leading to better treatment options. The technique, called near-infrared fluorescence lymphatic imaging (NIRFLI), has been developed at the University of Texas Health Science Center (UTHealth) at Houston Medical School in the US and was presented in a talk at the CLEO conference in San Jose at the beginning of June.
‘We really haven’t had any good way of imaging the lymphatic system and that’s a problem because many of the prevalent diseases that occur today – obesity, autoimmune disorders – are lymphatic conditions,’ explained Dr Eva Sevick at UTHealth and co-author of the paper.
The technology is being commercialised by NIRF Imaging in the US. The device uses a laser diode to excite a fluorophore – a trace dose of indocyanine green (ICG) in this instance – that is injected into the skin and is taken up by the lymphatics. Image intensifiers are then used to detect and multiply fluorescent photons, which are imaged with a CCD camera.
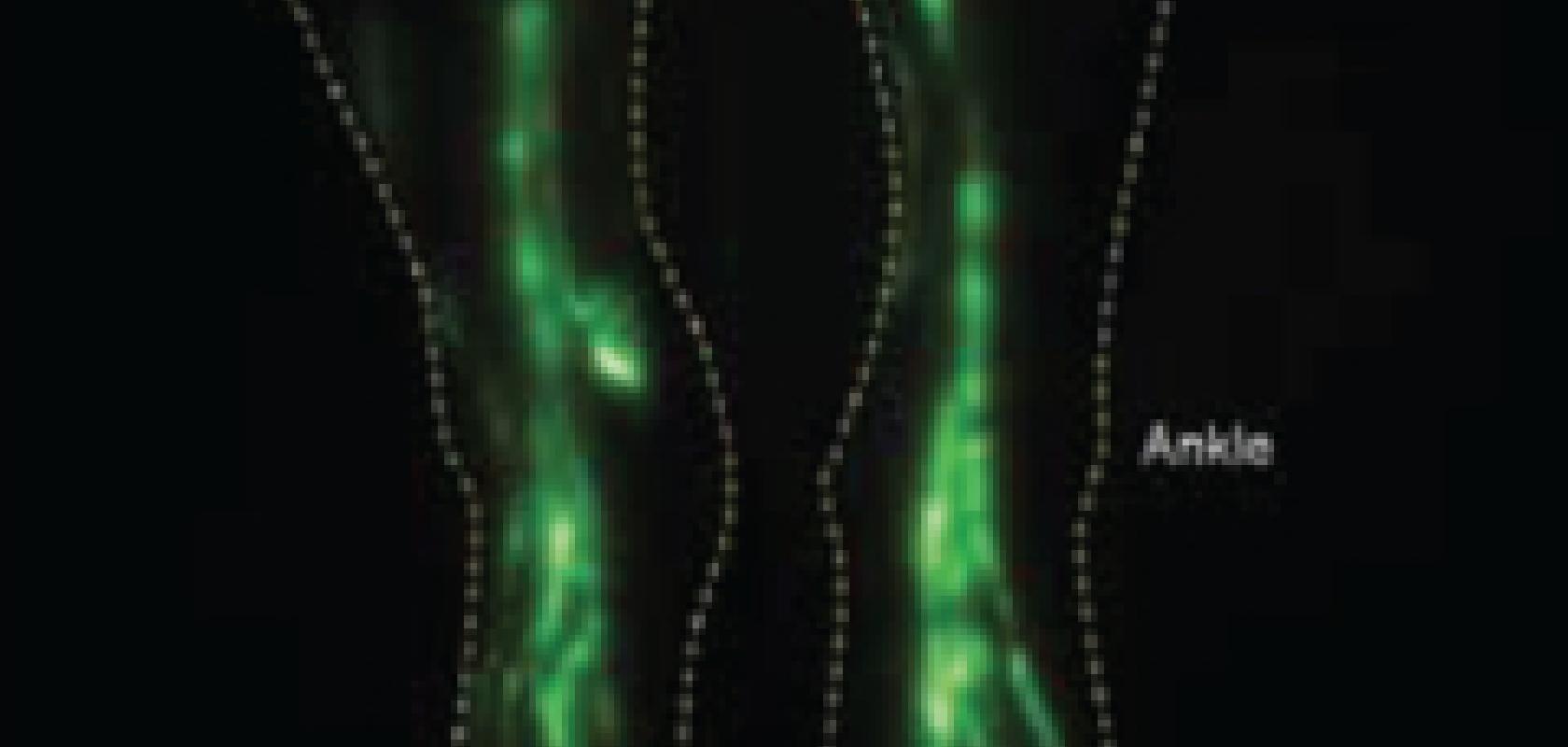
‘We’re able to acquire images of the lymphatics with high temporal and spatial resolution, depending on the measurement depth,’ said Dr John Rasmussen, also at UTHealth and co-author of the paper. The technology can also acquire a video of lymphatic flow to see how it functions.
The lymphatic system is a network of vasculature that picks up excess fluid draining from the arteries, veins and microcirculation and returns it to the blood vasculature. The fluid is called lymph – which, because it lacks any natural contrast, is difficult to image and doesn’t show up on CT or MRI scans.
In the western world, cancer survivors can get a condition called lymphoedema, in which, after lymph nodes are removed or the patient undergoes radiation therapy, an oedema, or build up of fluid, can form anywhere from months to years after cancer treatment. This affects about 20 per cent of all cancer survivors, said Sevick.
‘We have a hard time developing therapies for these diseases because we don’t understand how the lymphatics are involved,’ she said. ‘The only time people understood there was a lymphatic disorder is when the late-stage effects become apparent, such as irresolvable oedema. That’s too late. We can’t figure out what to do with these disorders because we haven’t had a chance to image them.’
In terms of treating lymphoedema in cancer sufferers, Rasmussen said that, if lymphoedema can be caught early, there’s a better chance of recovery. Waiting too long results in swelling that is more pronounced and the patient is disfigured. ‘Cancer tends to metastasise through the lymphatics and here we don’t know about the lymphatics because we haven’t been able to see it,’ said Sevick. The device is able to provide such detailed images with trace amounts of dye through a combination of the image intensifier technology and the optical design.
Sevick commented: ‘In nuclear imaging like PET, a radioisotope gives a single photon event and we have these beautiful 3D images. Here, we have a fluorophore that can give as many as 100 million photons per second per molecule. So, we should have exquisite sensitivity if we can develop devices that can detect these low-energy photons and reject the ambient light.’
The device’s ability to filter out ambient light combined with the detector technology means images can be taken every 200ms to produce a video of lymph flow. The lymphatic imager is expected to be available in 2015 through Nirf Imaging, and, unlike MRI, this will be a point-of-care device. ‘The technology will probably be applied first to evaluate cancer survivors first to see when we can detect the earliest signs of lymphoedema,’ noted Sevick.
The researchers are developing standards to certify the device performance. Sevick said: ‘If you buy a PET machine there are industry standards and phantoms for machine validation, but there are no industry standards for this type of medical imaging because it’s so new. A lot of scientists are putting camera systems together and developing new drugs, and the worry is they haven’t specified the performance of the device. So, if they fail to image anything, they might erroneously decide the imaging agent didn’t work when in reality the device probably wasn’t sensitive enough to detect it. We have a real problem in this whole area that we have to develop industry standards for this type of medical imaging.’
The group is also developing a new imaging agent for the device which they hope will enable cancer-positive lymph nodes to be imaged non-invasively, meaning the imager can be used during surgery in the operating room.
There are many other potential applications for this imaging technique, said Sevick: ‘We can see three to four centimetres deep – you can see an awful lot in the human body at this depth. There are a lot of applications – anywhere where nuclear imaging is used, there may be a counterpart for this near-infrared fluorescence imaging.’