A European research team has developed a handheld diagnostic scanner that can detect skin cancer in 30 seconds. It uses an infrared laser beam to identify blood vessels grown by malignant melanomas.
The devices could reduce the need for expensive and debilitating sentinel-lymph node biopsies while preventing patients having to wait weeks for a proper diagnosis.
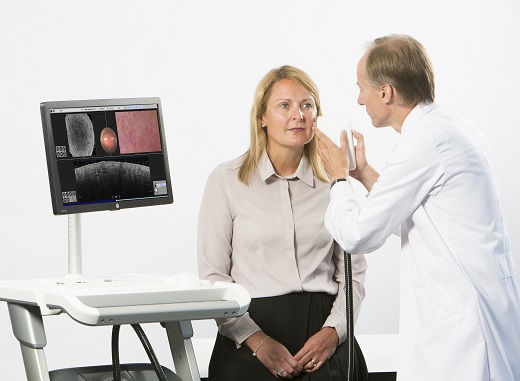
The 'VivoSight' scanner uses advanced OCT techniques to monitor the movement of blood vessels beneath the skin surface to detect skin cancer. (Credit: VivoSight)
The device, known as ‘VivoSight’, created as part of the ‘Automatic Detection of VAscular Networks for Cancer Evaluation’ (Advance) project, uses an infrared laser to create a 3D colour image of the blood vessels located nanometres under the skin via a new and advanced version of optical coherence tomography (OCT), a photonics technique more commonly used in retina scans. With it the device can identify the tell-tale distorted and malformed blood vessels produced by melanomas, allowing them to be used to confirm a cancer diagnosis in patients.
Being able to detect and see these vessels in real time has not been possible until now, according to the researchers, which opens the possibility of dermatologists making treatment decisions in previously unachievable timeframes.
Currently melanoma patients have to wait for a sentinel lymph node biopsy performed under general anaesthesia, which can take weeks to perform, is very expensive (around £10,000) and can be debilitating for the patient.
‘There has to be a better way,’ said the Advance UK project leader Jon Holmes. ‘Our scanner may radically improve the abilities of dermatologists to decide whether a melanoma is in the less malignant, non-spreading, early stage, or if it has already developed and requires immediate aggressive therapy. Further clinical trials will be needed to conclusively prove the technology.’
The variant of OCT used by the scanner is called ‘Speckle-Variance’ OCT or dynamic OCT (D-OCT), and is more suited to capturing movement than conventional OCT methods. The technique studies the ‘speckle’ or flicker of light patterns created by moving blood cells, taking around four images per second and compiling them to highlight what has moved between frames.
‘Using D-OCT we can see movement of blood against the solid tissue structures, something we have never been able to do before in a clinical setting,’ explained Holmes. ‘[Cancer] vessels are like twisty, branching country lanes that get narrower and wider. Our clinical team thinks that these “shapes” are key to understanding the cancer. Our scanner shows these vessels in gorgeous detail.’
As well as being used in skin cancer diagnosis, the ability to see blood vessel networks with the new scanner has created a number of useful spin-off benefits, according to the researchers.
‘The scanner can image the blood vessels in healing wounds,’ said Holmes. ‘This may have application for treatment of leg and foot chronic ulcers, when doctors want to know whether a wound is healing or requires a change in treatment, potentially reducing the number of amputations.
‘Advance technology may also help with burn victims, being able to give a doctor a quicker response time than the standard 15 days to determine whether a patient’s skin is healing and whether or not to give a skin graft.’
Coordinated in the UK, the Advance project received a grant of €2,282,143 from the European Commission’s FP7 programme. The project also involves participants from Germany, Denmark, Italy, and Serbia.

